CPAP Adherence and How to Improve It
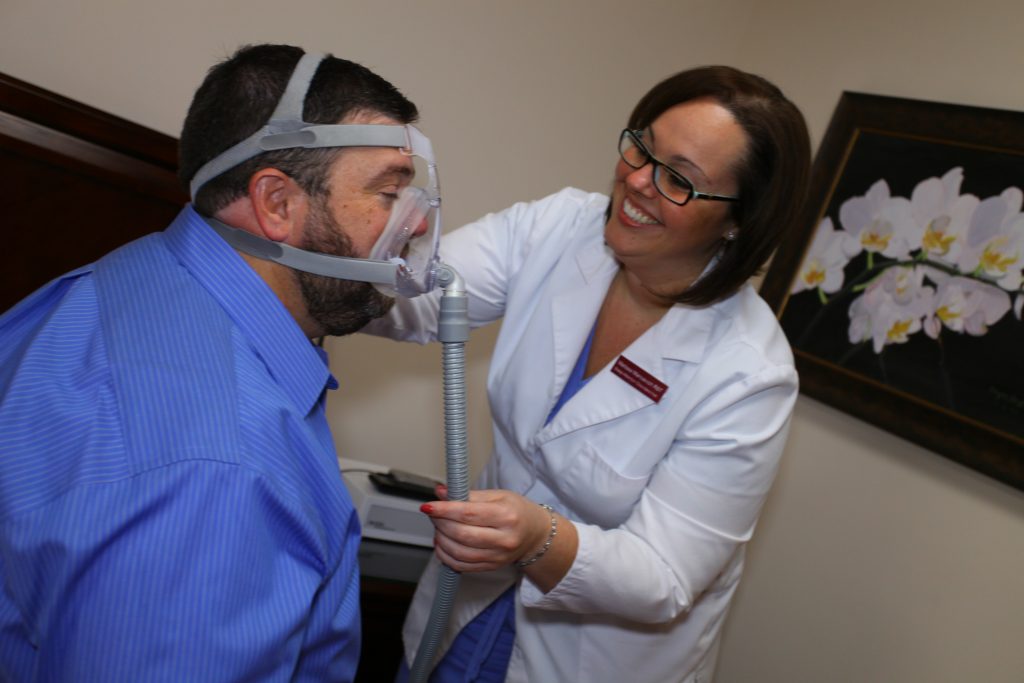
Continuous Positive Airway Pressure (CPAP) is the best treatment for obstructive sleep apnea (OSA). Unfortunately, only 59% of patients prescribed CPAP in the USA actually use it. Yet, being adherent to CPAP use is crucial in controlling OSA and its complications. The complications include sleepiness and fatigue, memory and concentration problems, high blood pressure, atrial fibrillation, heart attacks, strokes, and sudden death. At the Sleep Meeting in San Antonio in June, 2019, Dr. S R Patel reported that adherence is higher in older than in younger adults. Men are more adherent than women. Fewer patients are adherent in California and New York, and more in some Mountain states and some parts of New England. The Buffalo area has the lowest adherence rate. Patients who saw their primary care practitioner in the past year are more likely to be adherent.
How do we Improve Adherence?
Dr. N S Khan reported that four family engagement sessions with a caregiver and the patient did not change the proportion of patients who were adherent, although hours of use did increase. Dr. S I Patel found that peer support intervention does not increase adherence for the mentor. Dr. E M Beck found that cloud based care with phone calls at days 3, 7, and 14, followed by phone calls every 14 days for non-adherent patients until the 90th day, improved adherence from 53% to 66%.
Why is Adherence Important?
Dr. Terri Weaver reported that it takes 4 hours of regular use a night to improve sleepiness measured by sleepiness questionnaires. 40% of OSA patients have normal values on sleepiness questionnaires before treatment, 65% after 4 hours of nightly use. Using CPAP for more hours does not normalize the sleepiness questionnaire for more patients. On the other hand, for functional quality of life questionnaires, 30% of OSA patients are normal without treatment. 50% become normal after 7.5 h of nightly use. Using CPAP more seems to normalize a higher number of patients. Therefore, to improve sleepiness, you have to use the CPAP at least 4 hours a night. To improve functional quality of life, you have to use it at least 7.5 hours a night.
Patients who are more adherent to their prescription medicines are also more adherent to their CPAP. Partner engagement improves adherence, as do peer buddies. Motivational improvement nurse therapy also improves adherence. Patients who can define the risks of OSA, describe complications of OSA, and believe CPAP will help, are more likely to use it. Claustrophobia decreases adherence, but if patients keep trying, claustrophobia gets better. Patients, who regularly monitor their adherence, tend to use CPAP more.
I raised the point that side effects decrease adherence to any treatment. Therefore, it is important to correct the side effects. The side effect of CPAP with the second largest impact is arousals and awakenings. We know that CPAP adherence increases from about 60% to about 75% with the educational and supportive interventions mentioned by Dr. Weaver. I had shown that addressing arousals and awakenings with medicines such as trazodone, mirtazapine, and doxepin, further increases adherence to 90%. Dr. Weaver agreed that addressing arousals and awakenings was important.
I presented a poster showing what happens when patients on APAP who are having side effects with APAP, remain sleepy, or are non-adherent, are switched to CPAP. Adherence improves upon switch from APAP to CPAP, from 69% to 83%, and sleepiness improves further. Thus, CPAP works better than APAP in patients reporting problems with APAP or not responding to APAP. Patients with lighter sleep or worse desaturation were more likely to need a switch from APAP to CPAP.
Conclusion
CPAP works very well. However, it works only for patients who use it. Improving CPAP adherence is crucial. Educational and supportive intervention is important. Addressing side effects of CPAP, especially arousals and awakenings, is also crucial. We do all this, and adherence in our hands is 90%.









